Obesitas: patienten, läkaren och sjukdomen
En dag på läkarmottagningen, någonstans i Sverige
Tänk dig följande scenario: läkaren har patient på återbesök efter en genomförd lungröntgen. ”Här på väggen ser du din röntgenbild” säger doktorn. ”Vad tycker du..?”.
Patienten tittar en stund. ”Men… är det inte en fläck där? Ska den vara där?”.
”Vad bra att du säger det! Det kan vara en tumör”, säger doktorn. Sedan blir det tyst igen. Patienten säger till slut: ”Men kan man inte operera bort den?”. ”Jovisst kan man det”, säger doktorn. Åter tystnad. ”…men då vill jag nog det?” säger patienten försiktigt. ”Eller vad tycker ni är bäst?”.
”Operation är det enda sättet att rädda ditt liv”, säger läkaren så till slut.
Vad är det som inte stämmer i den här berättelsen?
Jo, rollfördelningen naturligtvis. Det är inte rimligt att patienten skall förväntas göra läkarens arbete -och i det här fallet kunde ju utfallet ha blivit katastrofalt för patienten, om denne inte ställt ”rätt frågor”. Om vi nu skulle påstå att en variant på just detta sker i princip dagligen i svensk sjukvård, hur skulle du reagera då? Vi hävdar att så är fallet inom vårt område -fetmasjukdom (obesitas).
Bakgrunden är denna: obesitas definieras som BMI >30 kg/m2 och drabbar i nuläget en miljon vuxna svenskar (referens 1). Fetmasjukdom förkortar generellt en människas liv med i genomsnitt 4 år, vid mer uttalad obesitas 5-20 år (referens 2, 3) och samhällskostnaden i Sverige är beräknad till cirka 25,2 miljarder SEK per år (referens 4). Trots detta visar enkätdata från patientföreningen HOBS bilden av att patientgruppen tvingas ”driva sitt eget case” gentemot sjukvården för att få adekvat vård -alltså en variant på vårt scenario ovan.. Exempelvis lägger sjukvården 15 gånger mer resurser på behandling av obesitas följdsjukdomar än på grundproblemet (referens 4).
Obesitas -en bortglömd sjukdom på våra vårdutbildningar
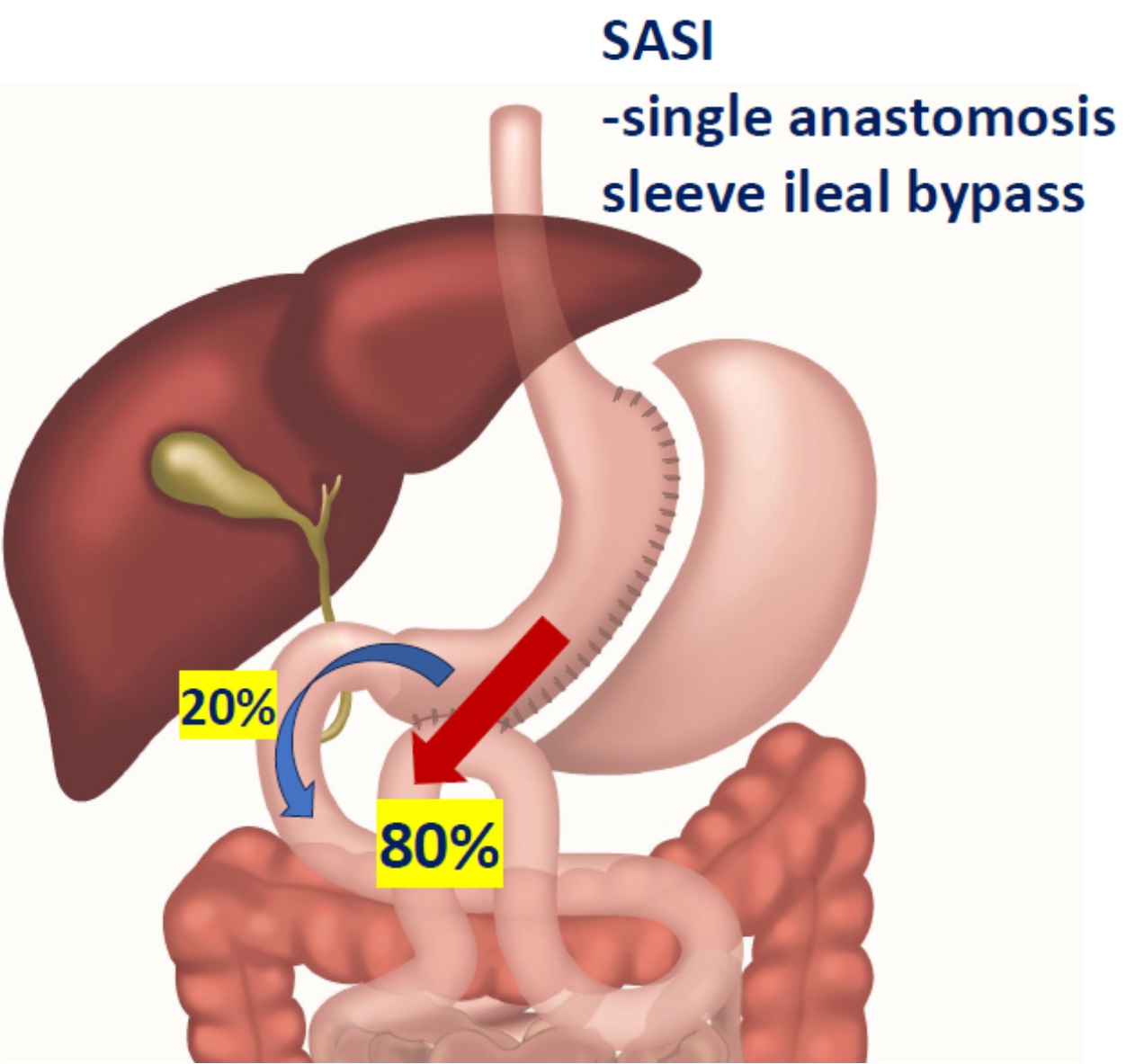
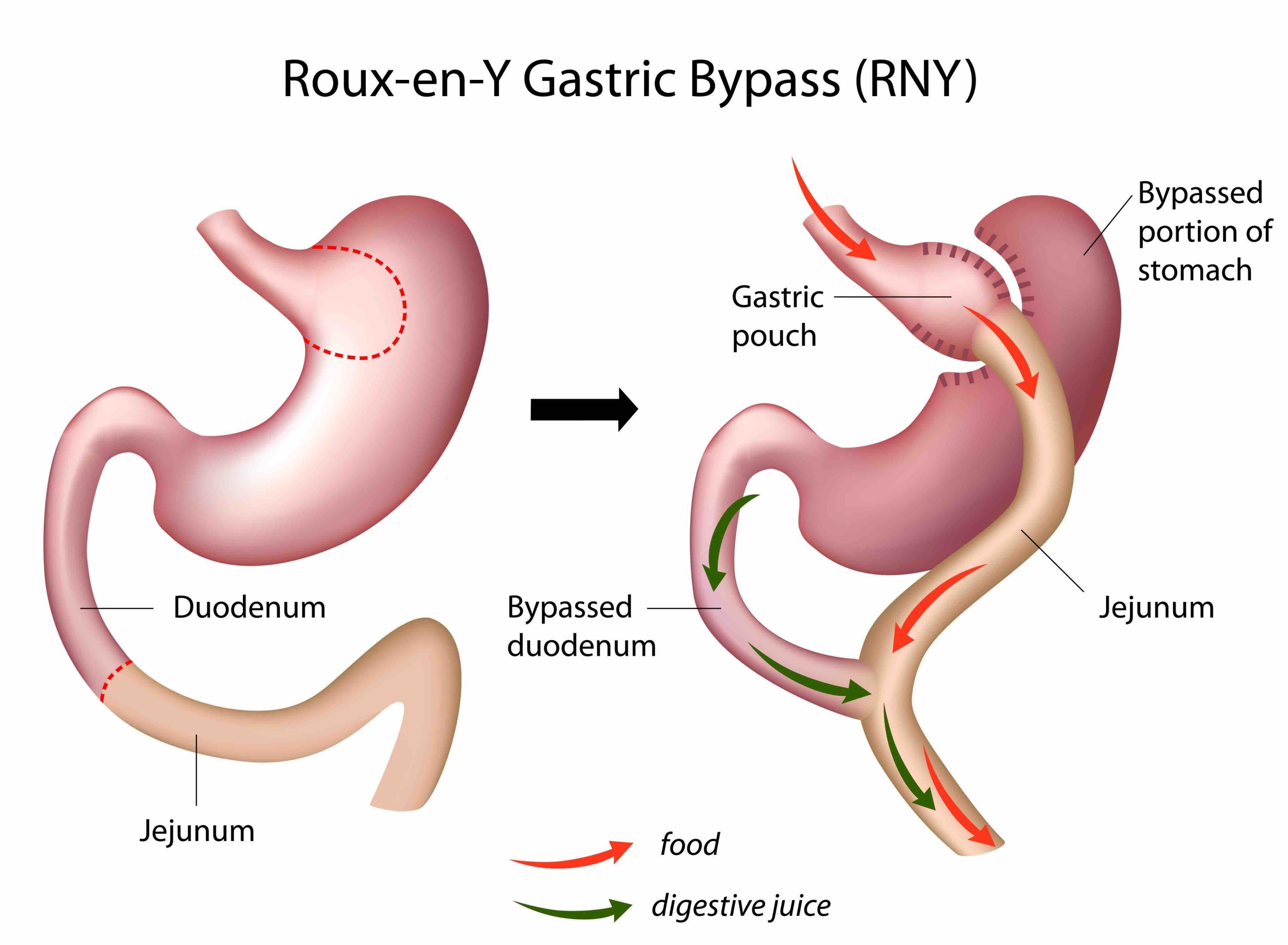
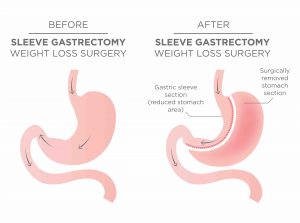
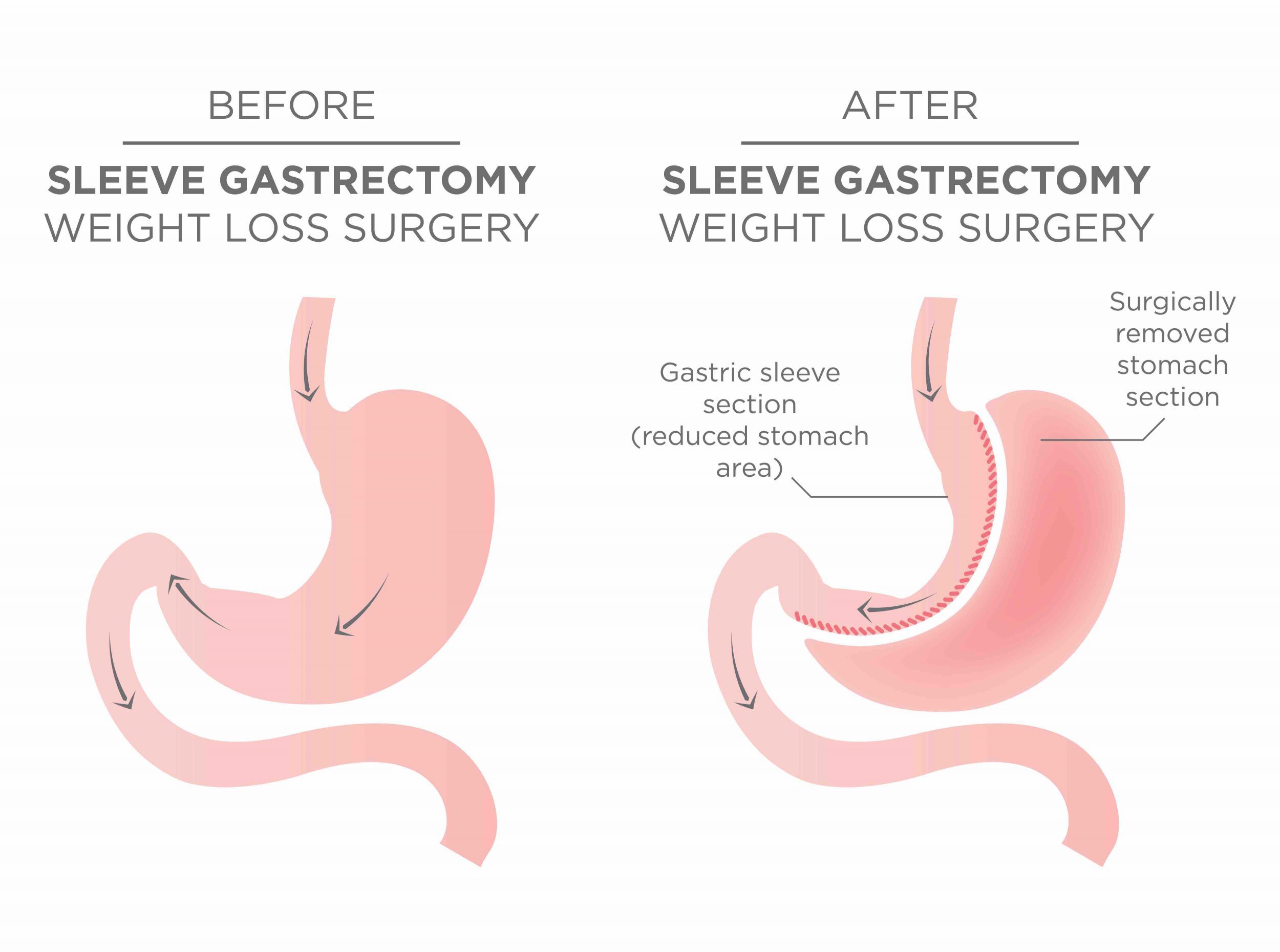
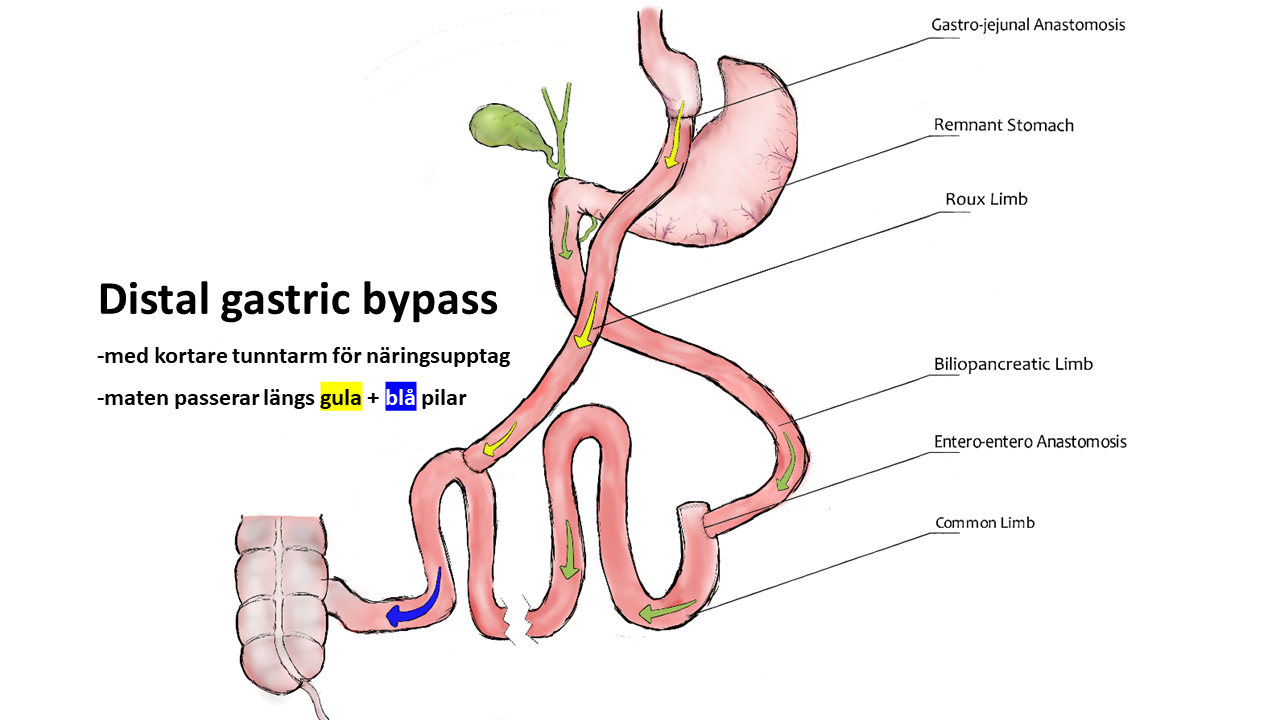
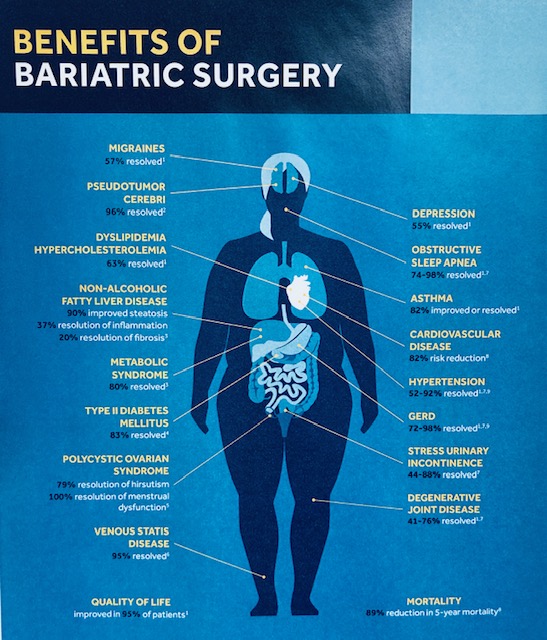
Samma typ av snedvridning ses inom vårdens grundutbildningar -den kroniskt biologiska sjukdomen fetma sorteras in under ”levnadsvanor” och kunskaperna kring kroppens viktfysiologi begränsas i princip till ovetenskapliga tankar om att helt enkelt ”röra sig mer och äta mindre” (vilket av biologiska skäl inte fungerar hos 95-97%). Den effektivaste evidensbaserade vården av uttalad fetmasjukdom är bariatrisk kirurgi –gastric bypass respektive sleeve gastrektomi i första hand. Hälsoeffekterna är dramatiska; exempelvis halveras förekomst av cancersjukdom hos kvinnor, genomsnittlig livslängd ökar med 6 år och samhället tjänar i storleksordningen 80000 kr per opererad patient i långsiktigt minskade samhällskostnader (referens 5, 6, 7).
Ändå är de offentligt finansierade operationsvolymerna i Sverige i stadigt sjunkande (referens 8) -och andelen egenremisser till bedömning inför fetmakirurgi är rekordhöga. Vad driver en patient till att skriva egenremiss, istället för att bli remitterad via sin ordinarie vårdgivare? Vi möts ständigt av patientberättelser där läkare dels i åratal undvikit att ta upp möjligheten kirurgi -men även många exempel på hur läkare aktivt vägrat att skriva remiss för att man ”inte tror på det där”. Nu kommer Sverige att ta fram nationella riktlinjer för en rad diagnoser, bland dem obesitas (referens 9). Detta kan på sikt förbättra den totala situationen för patientgruppen med obesitas. Samtidigt måste man vara realist -desto sämre generellt kunskapsläge inom ett område, ju sämre genomslag riskerar riktlinjerna att få.
Checklista för aktiv rådgivning om fetmakirurgi
Vi på GB Obesitas är ett expertcentra inom obesitaskirurgi. Vårt mål är att hjälpa såväl läkare som patienter att förstå när fetmasjukdomen är som fläcken på lungröntgenbilden i vårt scenario -situationer där det är direkt olämpligt att ur medicinsk synvinkel ignorera möjligheten av fetmakirurgi. En patient ska naturligtvis aldrig behöva driva sitt case själv -det är sjukvårdens uppgift att göra detta -men följande är att betrakta som de mest angelägna:
- BMI >35 och samtidig diabetes typ 2, evidens finns redan från BMI 30
- BMI >35 och samtidigt sömnapnesyndrom
- BMI >35 och samtidig symtomgivande artros på viktbärande led
- BMI >40 och PCOS med ofrivillig barnlöshet
- alla patienter med BMI >50 (i synnerhet män -det är farligare att vara man med obesitas än kvinna, ändå är bara 20% av de som opereras män).
Ovanstående checklista är såklart inte att betrakta som att man som patient skall tvingas till kirurgi -men man skall aktivt informeras om att operation är den effektivaste metoden för att bota ohälsa i det aktuella läget.
Har du som läser detta själv högt BMI och kanske passar in i listan ovan? Du bör du söka mer information -kanske operation är något för dig? Var gärna med på vårt nästa infomöte online!
Detta blogginlägg är en förlängd version av den debattartikel i Läkartidningen som bl.a. dr Broden hos oss var medförfattare till. Debattartikeln finner du här.
Referenser
1 Folkhälsomyndigheten, Livsmedelsverket. Förslag till åtgärder för ett stärkt, långsiktigt arbete för att främja hälsa relaterad till matvanor och fysisk aktivitet. Solna: Folkhälsomyndigheten, 2017.
2 Bhaskaran K dos-Santos-Silva I Leon DA Douglas IJ Smeeth L. Association of BMI with overall and cause-specific mortality: a population-based cohort study of 3·6 million adults in the UK. Lancet Diabetes Endocrinol. 2018
3 Fontaine KR, Redden DT, Wang C, et al. Years of life lost due to obesity. JAMA 2003;289:187-93. 10.1001/jama.289.2.187
4 Kostnader för fetma i Sverige idag och år 2030, IHE rapport 2018:3
5 Association of metabolic–bariatric surgery with long-term survival in adults with and without diabetes: a one-stage meta-analysis of matched cohort and prospective controlled studies with 174 772 participants. Nicholas L syn et al, The Lancet VOLUME 397, ISSUE 10287, P1830-1841, MAY 15, 2021
6 Effects of bariatric surgery on cancer incidence in obese patients in Sweden (Swedish Obese Subjects Study): a prospective, controlled intervention trial. Sjöström L et al. Swedish Obese Subjects Study. Lancet Oncol. 2009 Jul;10(7):653-62. doi: 10.1016/S1470-2045(09)70159-7.
7 Cost-utility analysis of bariatric surgery compared with conventional medical management in Germany: a decision analytic modeling. Oleg Borisenko et al. BMC Surg 2017 Aug 3;17(1):87. doi: 10.1186/s12893-017-0284-0
8 Svenska obesitaskirurgiregistret SOReg
9 socialstyrelsen.se/regler-och-riktlinjer/nationella-riktlinjer/pagaende-riktlinjeprojekt/fetma/









Senaste kommentarerna